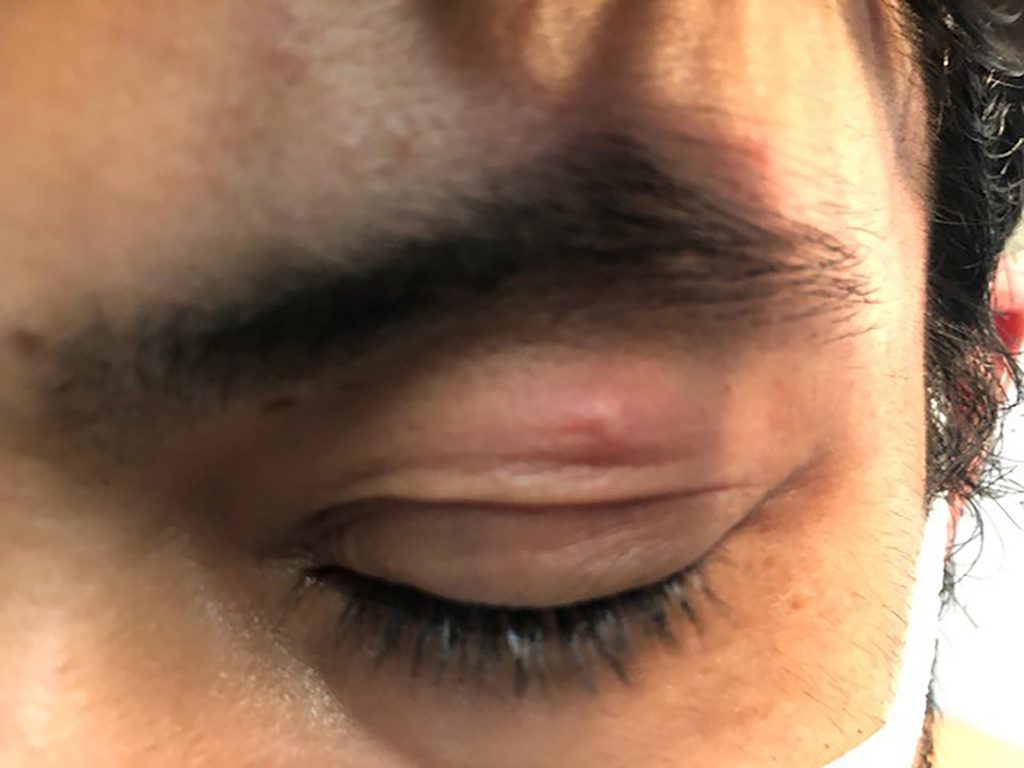
Keratitis of the left eye in a 36-year-old cisgender man with HMPX, imaged at lesion day 2.
Nontender, nonpruritic erythema of the left bulbar conjunctiva with copious watery discharge associated with mild visual blurring. Ophthalmopathy examination revealed dendritiform changes on the cornea, suggestive of a viral etiology; PCR of a conjunctival swab was positive for MPXV. This was associated with other mucous membrane involvement in the form of pustules and ulcers on the inner lip and soft palate and pharyngitis, all of which developed on illness day 7 along with several cutaneous lesions across the face, scalp, torso, genitals, and bilateral upper extremities.
Given nonresolving keratitis after 14 days, he was treated with a 14-day course of twice daily oral Tecovirimat and Prednisolone 1% ophthalmic drops instilled four times daily. Only mild erythema and blurry vision remained 3 days later, which resolved by follow-up 9 days into treatment.
There was no history of immunocompromising conditions or medications. This man was on Truvada for HIV pre-exposure prophylaxis.